#how can a slow lung choose a respirator? # chronic obstructive pulmonary disease (slow obstructive lung, copd) is a sexually irreversible respiratory disease that is often accompanied by chronic respiratory failure at a later stage, in the form of symptoms such as respiratory difficulty, inactivity, and awakening at night, which seriously affects the quality of life. Respirators, as core breathing support equipment, are effective in improving pulmonary aerobic function, ejecting carbon dioxide and increasing blood oxygen saturation, subject to the patient's medical condition, use of scenes and physical tolerance scientific choices. The following are the key elements of the streamlined core guide, balancing practicality with professionalism。
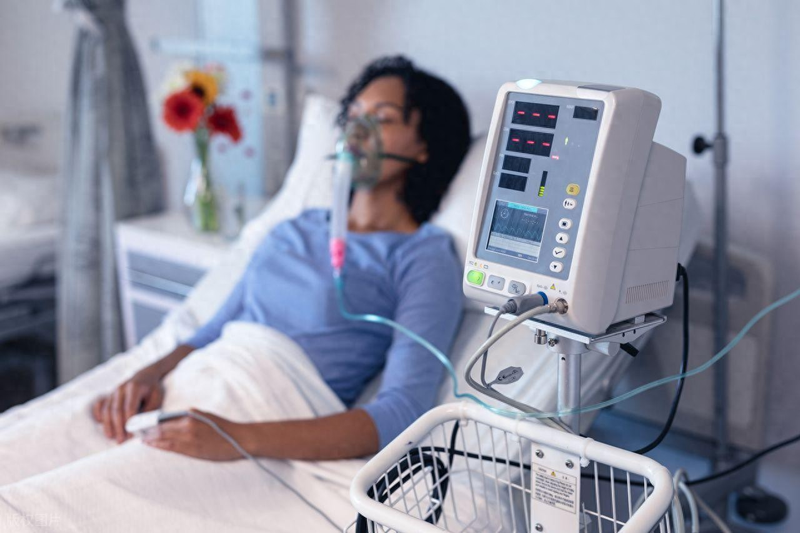
I. Applicable population groups (doctoral precision assessment): not all patients with slow-retarded lungs are required to use respirators, with three categories of core applicable population:
1 for patients with severe/extremely severe slow lung resistance, i. E. A first-second excretion volume (fev1) < 30% expected, or associated with chronic respiratory failure (paco2=50mmhg, aerobic pressure pao2<60mmhg) with prolonged oxygen treatment
2. Patients with chronic respiratory retardation during acute stress periods, severe respiratory distress and acute respiratory failure, require short-term ventilation to support the passage of critical periods; and patients with “overlapping syndrome” that suspends low permeability through combined sleep breathing, which exacerbates lung damage and requires nighttime ventilation。

(ii) mechanical choice (priority, suitability): home-based use of non-respiratory devices is the preferred option, and hospital serious conditions require a respirator (no home-based purchase)。

There are two types of breathing machines:
1. (bipap): preferred machine type for slow-retarded lung patients, which independently regulates the inhalation phase pressure (ipap) and the exhalation phase (epap), boosts the boosting capacity to ventilate when inhaled, safeguards the collapse of the gas route when inhaled, improves co2 retention with precision and corresponds to a majority of patients who combine respiratory failure
2. Single-level positive-pressure respirator (cpap): provide only constant pressure, simple operation, pro-people prices, but limited improvement in carbon dioxide sequestration, recommend only those who are used for overlapping syndrome and slow to resist lung symptoms, and do not recommend first choice for patients with simple respiratory failure。
Iii. Core elements of the selection:
1. Strict adherence to medical guidance: the carrying of medical records such as lung function reports, blood and gas analysis, and the identification by doctors of mechanical and preliminary parameters to avoid blind selection
2. Focus core performance: priority is given to the type of machine that is synchronous (e. G. Avoiding human confrontation), pressure stability (floating 1 cm h2o), noise 30 db (not affecting sleep), with a thermo-moistor (protecting airways), with a four-hour portable package of selected weights to be used by the outsider
3. Optimal formal branding: selection of brands with medical equipment registrations (e. G. Philips, reisma, fish jumps, etc.), confirmation of sale with home installation debugging, 24-hour hotline and 1-2-year quality assurance
4. Suitable mask/nose mask: nose mask suitable for a normal nasal cavity, mask suitable for an oral breather, preference for silica glyphs, size by facial profile, avoidance of leakage or skin pressure。
Iv. Use and maintenance norms: the parameters are strictly medically prescribed and cannot be adjusted; four hours per day are recommended for use of thorium, better use during night sleep, immediate suspension and counselling are required in case of discomfort, dizziness, serious leaks in the mask, etc.; daily maintenance is required: the wetter is only free of bacterial water, the mask is cleaned daily, 75 per cent alcohol is sterilized every week, respiratory filters are replaced once a month, equipment is placed in a dry ventilation area to avoid direct sunlight。
Core principles: people with slow lung resistance need to adhere to “medically appropriate priorities, reliable performance to complement and standardized use of respirators”. Scientific choices and the correct use of respirators can effectively mitigate symptoms, slow progress and significantly improve the quality of life of patients。
# slow lungs #




