What about cpr and heimrick? How does aed work? Cardiac arrest, gastrophagus, heat, drowning, electrocution, burns... 6 major categories must have a collection of first aid knowledge that you cannot use, but you must know. World red cross day, functional transfer

"four minutes of gold."
Early cpr and aed are critical to improving success and prognosis
What about cpr
On-site adult cpr operation process
If a sudden fall is found, the rescuer needs to confirm that the environment is safe, to protect himself, to judge the patient's consciousness and reaction and to examine the breathing. If the patient is unconscious and unable to breathe, call immediate help, call the emergency number and get an aed and start cpr as soon as possible:
One chest pressure
The rescuer first exposed the patient's chest, with one hand close to the patient's chest, the middle point of the two nipples line (lower part of the chest), with two hands tied together, with three hands in each other's hands, one hand in each other's hands, one hand in each other's hands, one hand in each other's hands, one hand in each other's arms, two arms in the upper body, one body in the upper part, one in the upper part, one in the upper half, and one in the upper half. Press the pressure straight down to ensure that the pressure depth is 5-6 cm and the pressure frequency is 100-120 times/min, and that the post-pressure chest profile is fully restored at each time。
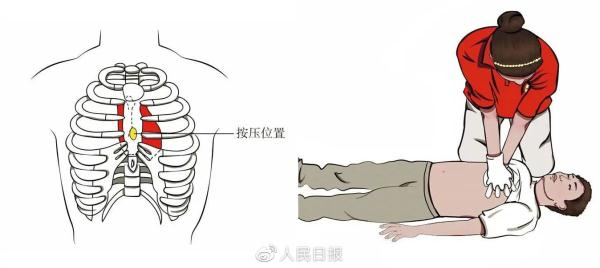
2 open airways
Check for foreign objects and remove them if they exist. Open airways with hindsights, usually vertically linked to the horizontal surface of the patient's jaws and earlobes。
3 artificial breathing
The rescuers covered the patient's mouth with their fingers, squeezed the patient's nostrils, and blew twice, each time for about one second, with the chest contour rising。
4 cycles for extra chest pressure and artificial respiration
Circulatory 30 ecstasy pressure and 2 artificial respirations (30:2) with a 5-group assessment of the patient's breathing and pulse。
Electron defibrillation as soon as possible
How do we use the life savior aed
One on aed
Open the package, remove the aed, turn on the power switch and act on the voice alert。
2-pilot emp
Position of adult electrodes:
According to the image on the aed electrodes, one electrode is attached to the top right of the patient's naked chest (right side of the chest, under the collarbone) and another to the outside of the patient's left nipple (the fifth rib after the front line)。
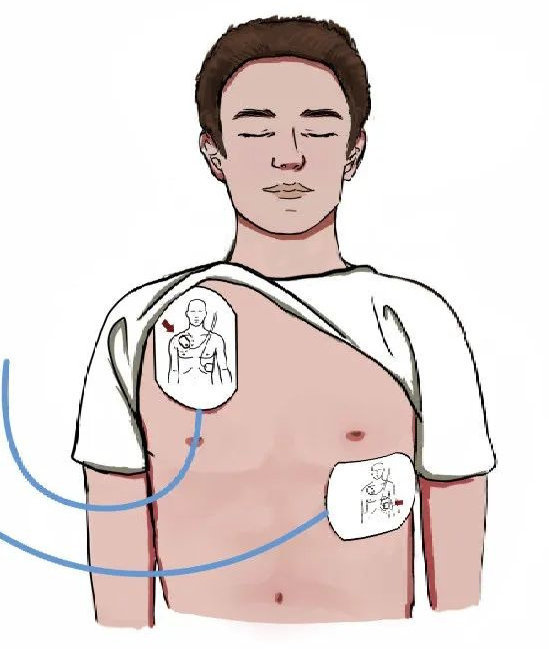
Location of infant and child electrodes:
Two electrodes are attached to the chest and the left shoulder of the baby and the child, respectively, and larger children can also place electrode as adults。
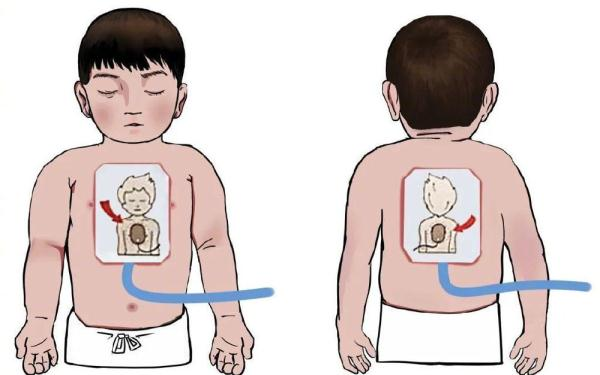
3aed analyzes the heart rate
When aed analyzes the heart rate, the language of the rescuer suggests that people around them should not be exposed to the patient and shouts, “please do not be exposed to the patient”, waiting for aed to analyse the heart rate to determine whether electroshock is required to defibrate。
Four shock defibrillation
If aed recommends defibrillation, it needs to be reconfirmed that all persons have no contact with the patient。
When aed is fully charged, press the “shock” button to discharge or aed automatically defibrate。
If the aed suggests that no electroshock defibrillation is required, cpr should be implemented immediately if necessary。
Continue cpr after 5 defibration
The cpr continued immediately after the electroshock was removed. In two minutes, aed will automatically analyse the heart rate again to determine whether further tremors are required. This is repeated until the patient recovers his or her heart and breathing, or the arrival of a specialist first aid worker。

The identification of aerobic alien objects is key to the success of the rescue, and patients are often automatically attached to their neck and throat with one hand or both, known as the “v” gesture。
Light air-traumatization symptoms should encourage patients to cough hard and try to extricate。
Severe air-traffic obstruction symptoms, but conscious, should immediately call the first-aid telephone and do so in the following ways:。
Adults and children
1. Back prostration
One of the rescuers stood behind the patient, supported the patient's chest with one hand, leaning forward (with the back bending forward) to the advantage of the alien being removed from the mouth rather than falling in the respiratory tract。
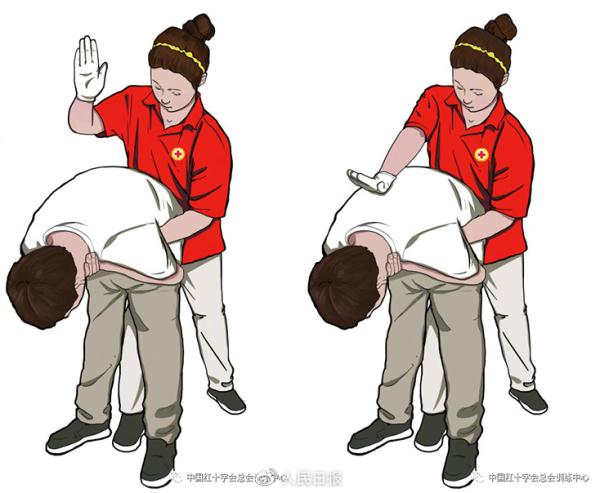
2 5 times with the hand of the other hand in prostration between the patient's shoulder cheekbones。
After each cropping, check that the air-traffic barrier is lifted and, if lifted, do not have to be completed five times。
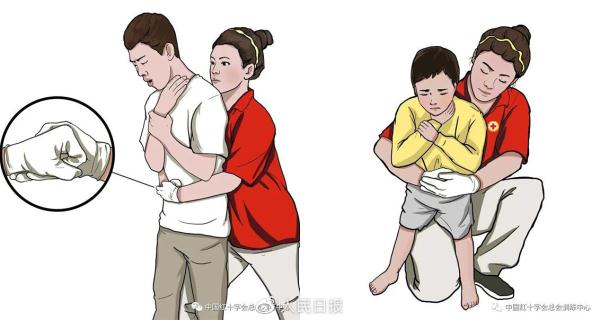
2. The abdominal impact method (heimrick first aid)
1 the abdominal shock is carried out immediately when the back prostration does not remove the aerobic barrier of the patient。
The rescuers stood behind the patient or kneeling on one knee behind the sick child, surrounded by arms around the patient's waist and leaning forward。
The savior held a fist with one hand, held a thumb side of the fist against the patient's sword and belly button (both fingers on the umbilical cord), and the other held the fist tight, punching hard inwardly and upwards five times。
Following each abdominal shock, check that the air-traffic barrier has been lifted and, if lifted, do not have to be completed five times, and if not, continue to perform five back prostrations in rotation。
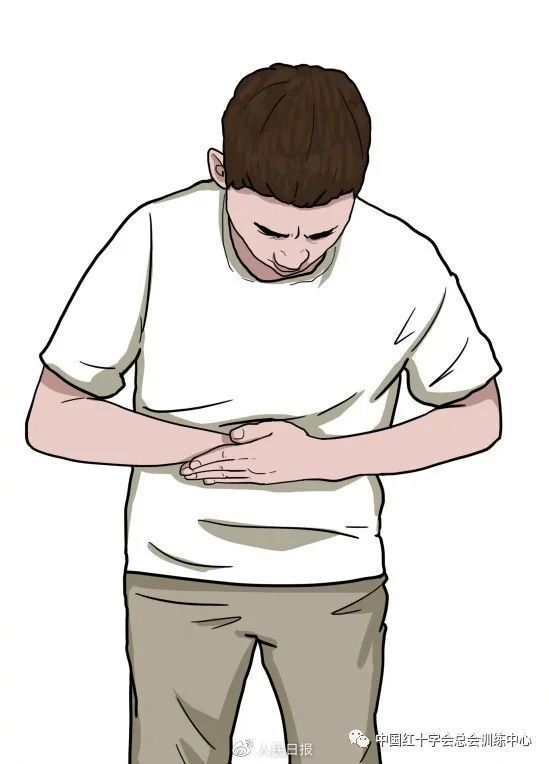
3. Self-help abdominal shocks
Self-saving abdominal shocks can be used when there is no help at the scene and telephone calls are difficult to report。
One patient holds a fist with one hand and closes his thumb against the sword between the bowels (two fingers on the umbilical cord)。
The other hand held the fist tight and hit it up and inside。
The option is also to place the upper abdomen on a hard plane, such as the back of the chair, the table edge, the corridor rail, etc., bending over and continuously impacting inwardly and upwards until the alien is released。
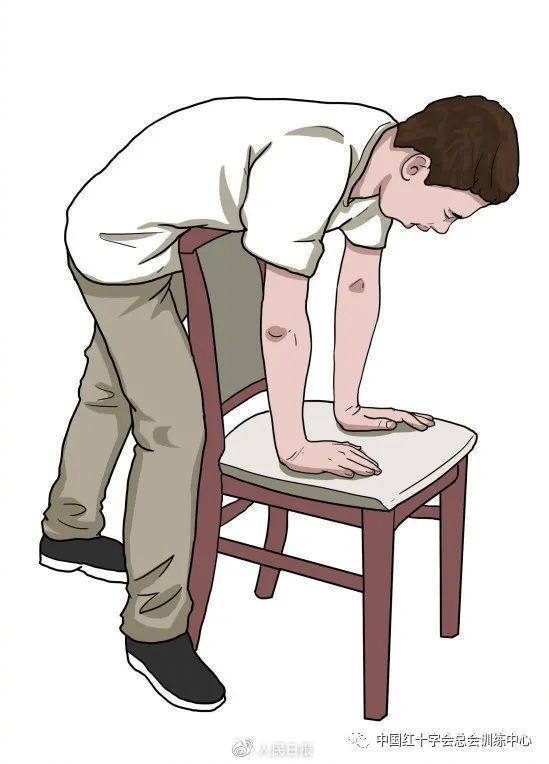
I'll make a sketch of it
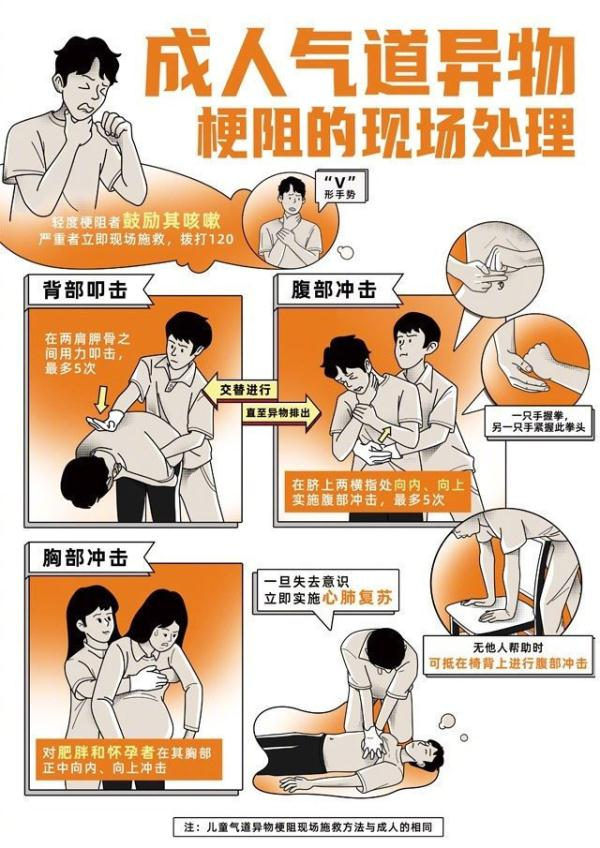
Baby
1. Back prostration
A rescuer sits or crouchs, holds the baby up, protects the baby's neck with one hand and places his head on his forearm。
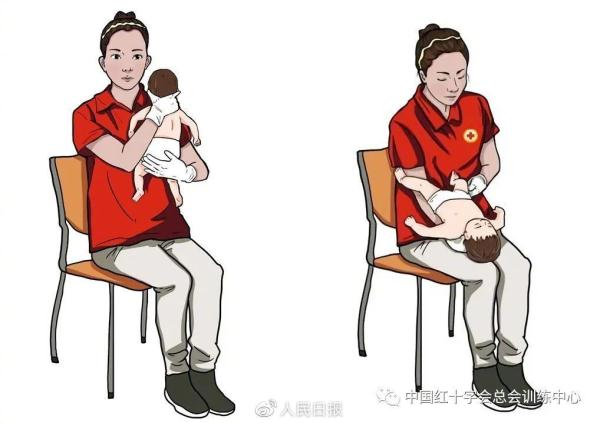
The other hand fixed the baby's lower jaw, slashed the head back, turned the baby into a tumbler, putting it down on the arm of the healer and down to the body。
The rescuers used the palm of one hand to bow five times between the child's shoulder cheekbones。
After each bowing, check whether the air-traffic barrier has been lifted and, if lifted, no more than five times。
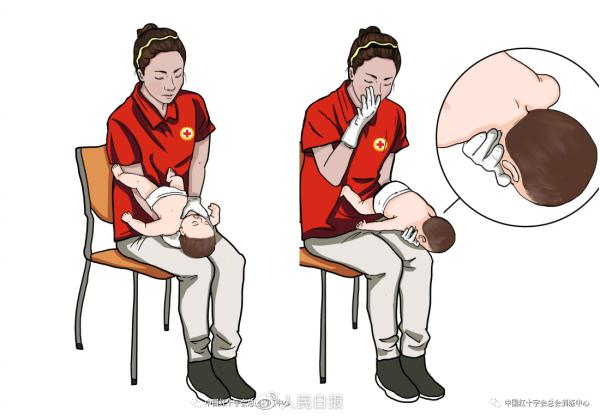
2 the chest shock method
The chest shock method is immediately enforced when five back prostrations do not remove the aerobic barrier of the baby。
A rescuer sits or remains in a position where the baby is fixed with two hands and a forearms, which is turned to a recoil, keeping the baby in the direction of the rescuer's arm, with its head down (or lashing) on its thighs。
2 rescuers apply a middle finger and an anonymous finger (or an index finger) from one hand, with a vertical downward pressure on the baby's chest in the middle and below the two nipple line, five times, at a depth of about one third of the baby's chest diameter。
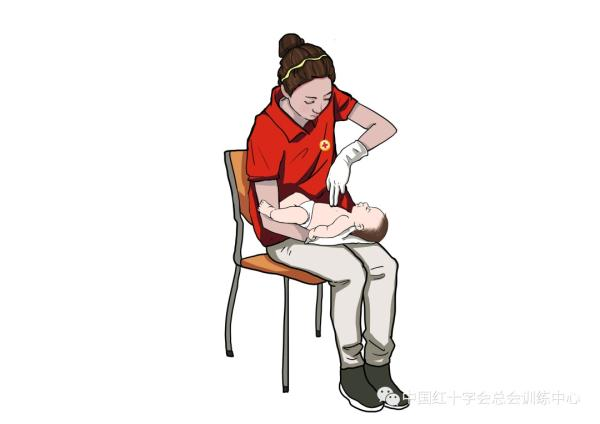
Following each shock, check that the airway barrier has been lifted and if it is lifted, do not have to be completed five times, and if it is not lifted, continue to perform five back prostrations in turn。
Note:
To avoid blind use of fingers to clean out the respiratory tracts, such as the presence of visual objects in the baby's mouth, which can be cleared by a small finger。
After the removal of the aerobics, even babies who appear to be in good condition should be examined at the hospital as soon as possible to ensure that there is no damage to the aerobic or other internal organs。
Once the baby is unconscious, it is carefully moved to a hard plane; if no first aid call has been made, it is called immediately; and the airway is opened and given two to five artificial breathings, followed by cpr。

When in high temperatures and wet conditions, when there are symptoms such as sweat, thirst, indigence, eyeslids, nausea, headaches, dizziness, etc., the heat must be kept on guard。
1 the patient is immediately transferred to a low-temperature environment, such as a cool, ventilated or air-conditioning room, where he or she is unbuttoned, untied or undressed。
(b) do not rush to replenish large quantities of water with salty or salty drinks。
The temperature is increased by cold dressing, bathing the whole body (to remove the chest), while the wind accelerates the dissipation of heat, and colds the lower parts of the armpit, neck and groin with ice bags。
In serious cases, call 120 or take them to hospital immediately。

Five principles for ashore rescue
Once rescued, no water control is required。
As far as possible, the drowning has been placed in a side wing to keep warm。
If the drowning person is unconscious, clean up his nose and mouth quickly and keep his airways open。
If the drowning person's heart stops, he or she takes two or five artificial respirations, followed by an extra chest pressure。
Do not give up the rescue of the drowning。

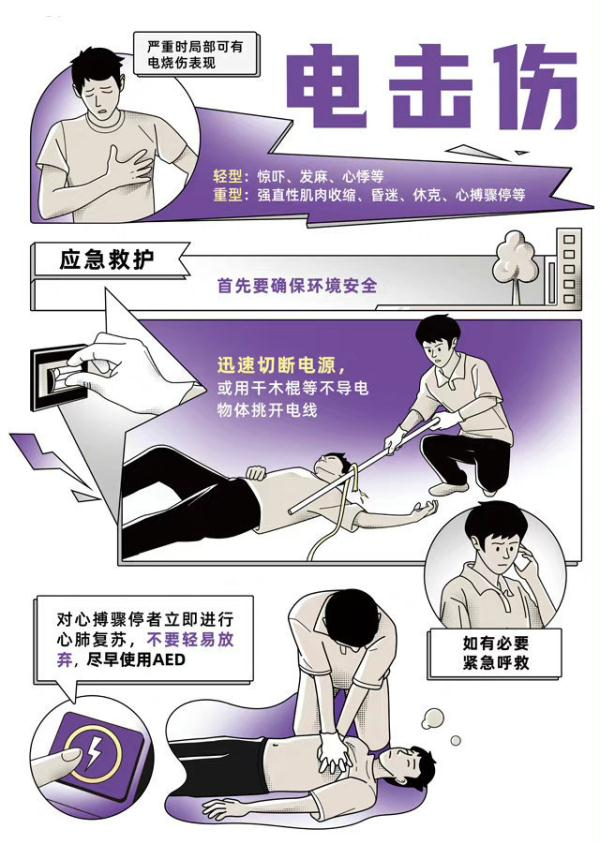
The power should be cut quickly and the electrocutor removed from the power as soon as possible. I'm sure i'm safe from electrocution。
Two electric shock injuries are most likely to cause a cardiac arrest, which is quickly examined when the patient is removed from the power supply. The patient has no consciousness, breathing, burns, etc. If the patient is unconscious and breathing, he/she must compete for seconds for cpr. Called “120 immediately”, the first aid doctor arrived at the scene and was escorted to the hospital for further first aid in the event of uninterrupted rescue。
3. After being removed from the power source, the minor electrocutor shall rest in situ for between one and two hours before moving. There is no danger to life, and burns and wounds are covered with clean gauze or clean cloth, and trauma is treated。

Burn classification and performance
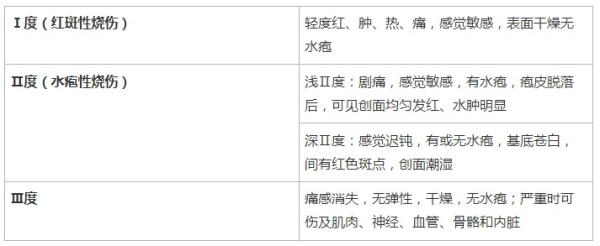
Temperature from cold water (15-25°c) is immediately and continuously washed (or immersed) until pain is eased; ice is avoided, especially when the area of the burns is larger (20% or more). If necessary, the emergency system is activated by urgent calls。
The clothes of the wound must be removed or cut off quickly, and they must not be removed from force or removed。
I-degree burns can be used with external burn ointment, which is usually cured from 3-7 days。
(b) second degree burns, no puncture, no ointment on the surface, and the application of clean dressings (such as gauze, towels, etc.) to cover the wound (as far as possible without the use of hair-prone fabric) in order to protect the face, prevent infection and bring it to medical attention immediately。
For severely thirsty persons, a small amount of salt water or salt tea may be oral. Burning beverages are available when available。
Hemorrhage should be stopped when accompanied by external haemorrhage; fractures should be temporarily fixed。
Persons with extensive or severe burns should be referred to hospitals as soon as possible。